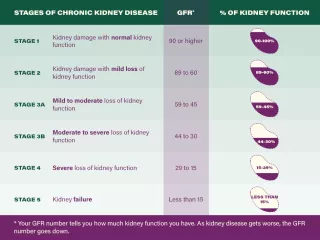
Chronic Kidney Disease and Racial Disparities in Healthcare
The Barriers
The higher number of Black Americans with kidney failure compared to the lower number of White Americans with kidney failure is a gap or health disparity. A health disparity is the difference in quality of care or health outcomes for a nonminority group compared to a minority group.
Barriers to Transplant Access
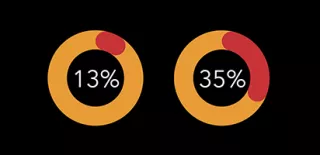
Black Americans with kidney failure have lower access to transplantation. While Black Americans account for 35% of people receiving dialysis, they are less likely to be identified as kidney transplant candidates compared to White Americans. Black patients with kidney disease often encounter barriers throughout the steps to transplant access. They have to wait a year longer on average than white patients to receive a kidney transplant.
Eligibility
Black patients with late stage CKD often are not identified as eligible for transplantation. A contributing factor, recently addressed by the medical community, was inequity in eGFR calculation. Researchers found that about 1 out of 3 Black patients with late-stage CKD had been classified incorrectly in a recent population-based study. Eliminating this inequity in calculation will improve access to appropriate, timely care.
Referral
The most significant barrier to kidney transplantation is timely referral for evaluation. Patients must have an evaluation to be recommended for a kidney transplant.
There are many benefits to early referral. Early referral allows patients
- Access to the waitlist before starting dialysis
- More time to look for a potential living donor
- More time to receive education about transplantation
- More time to complete a transplant evaluation
- Access to a kidney specialist
Black patients are less likely than White patients to be referred for transplantation. Patients from Black communities who are receiving dialysis are less likely to be referred to a nephrologist before beginning dialysis.
Medically appropriate patients should be referred for evaluation once an eGFR of less than 30 mL/minute is reached. In an analysis of one US healthcare system, even when 64 Black patients were reassigned to an eGFR of less than 20 mL/minute, none were referred for kidney transplant.
Evaluation completion
It is difficult for many patients to complete an evaluation required for recommendation for kidney transplantation. Transplant evaluation requires many trips to healthcare facilities. Patients typically meet with a transplant nephrologist, transplant surgeon, transplant coordinator, social worker, and psychologist. They also may meet with a financial coordinator, pharmacist, and dietician. The patient must undergo several tests, including cardiac testing, chest x-rays, blood tests, routine health screenings (eg, mammogram, colonoscopy), and a dental examination. Other testing may be needed based on the patient’s medical conditions.
Attending all of these appointments requires time off from work as well as transportation to and from the facility. Sometimes workers have no paid sick leave. For those who earn hourly wages, going to medical appointments instead of going to work creates financial stress. Patients who live in rural areas may find it difficult to travel long distances for multiple appointments. In many cases, transportation is not available.
Women have particular challenges as primary caretakers for children, elderly, or ill family members. Taking care of their own needs creates gaps in care for loved ones.
Waitlist
Black patients are less likely than White patients to gain access to a waitlist for transplantation. One barrier is that many transplant centers have a Body Mass Index (BMI) requirement. This can limit kidney transplant as an option for overweight patients.
Transplant
Black transplant candidates wait longer than White transplant candidates for kidney, heart, and lung transplants and have less access to both living donor and deceased donor transplants. The greatest disparity exists in access to living donor transplants.
Historical Impact of the eGFR Race Correction
In the past, the eGFR race correction multiplier was used in formulas to calculate how well the kidneys were working. In 2021, the National Kidney Foundation and American Society of Nephrology recommended a new approach to eliminate this inequity.